
At the office of Riverbend Family Dental, our aim is always to preserve natural teeth whenever it’s safe and sensible. Still, there are situations when removing a tooth is the most responsible step to protect your oral health, comfort, or overall wellbeing. We approach every extraction with careful planning, explaining the reasons, the process, and the options that follow.
Deciding to extract a tooth is a clinical judgment based on a thorough exam and a clear understanding of your medical history. Our team evaluates the tooth’s structural condition, the surrounding bone and gum support, and how the problem affects neighboring teeth and bite function. Where appropriate, we’ll review alternatives and why extraction is recommended for your specific case.
We place a high priority on patient comfort and clear communication. Before any procedure, we discuss anesthesia choices, expected recovery, and potential next steps for replacing a missing tooth if that’s part of your long-term plan. This helps you leave our office feeling informed and confident about the care you receive.
Delayed or problematic baby teeth
Sometimes a primary (baby) tooth does not loosen and fall out as the permanent tooth beneath it begins to erupt. When a baby tooth remains firmly attached—due to undeveloped root resorption or fusion to the jawbone—it can block the normal path of the adult tooth and cause alignment issues. Removing an over-retained primary tooth can allow the permanent tooth to emerge properly and support better long-term alignment.
Extensive decay that can’t be restored
Tooth decay can start small but progress deeply into the enamel and dentin, sometimes reaching the nerve and weakening the tooth’s structure. When the damage leaves insufficient healthy tooth to anchor a crown or other restoration, extraction may be the safest option to prevent ongoing infection and pain.
Severe fractures or cracks
Teeth that have been badly fractured, especially when the break extends below the gumline or compromises the root, may not be salvageable. In those situations, removal reduces the risk of persistent pain and recurrent problems and can set the stage for effective replacement options.
Advanced periodontal (gum) disease
Longstanding gum disease can erode the bone and soft tissue that stabilize teeth. When a tooth has lost significant support and becomes loose or painful, extraction can stop further damage and help stabilize the overall health of the mouth.
Wisdom teeth that cause trouble
Third molars often erupt without room to fit comfortably. Impacted or improperly positioned wisdom teeth can cause decay, crowding, cysts, or harm to adjacent teeth. Removing problematic wisdom teeth when indicated prevents future complications and can protect oral health.
Orthodontic space considerations
In some orthodontic plans, removing one or more permanent teeth creates the space needed to align teeth and achieve a stable bite. Extractions performed for orthodontic reasons are carefully planned in coordination with your overall treatment goals.
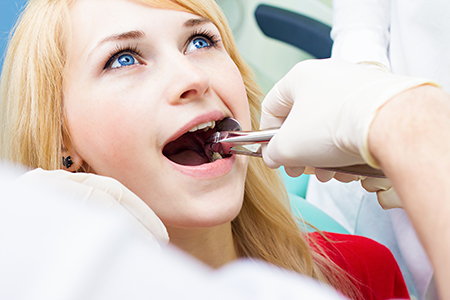
Every extraction begins with a focused review of your medical and dental history so we can tailor care to your needs. Please tell us about any prescription medications, over-the-counter drugs, or health conditions you have—these details help us plan anesthesia, consider antibiotic precautions when necessary, and coordinate care with your primary physician if required.
We use conventional diagnostic tools such as a clinical exam and digital X-rays to see the tooth and its surrounding structures. Imaging helps determine whether a tooth is straightforward to remove or if a more involved surgical approach will be needed. We’ll explain the anticipated technique and answer your questions so you know what to expect.
Managing anxiety, pain control, and safety are priorities. Most extractions are completed with a local anesthetic that numbs the site. For patients who need additional support, we offer sedation options to reduce fear and ensure a calm, controlled experience. Aftercare instructions are provided in detail to support healing and minimize complications.
A simple extraction is performed when the tooth is fully erupted and visible in the mouth with a root structure that is reasonably straightforward. After numbing the area, your dentist gently loosens the periodontal ligament and removes the tooth using forceps. The procedure is usually quick, and recovery tends to be uncomplicated with standard post-operative care.
If you feel nervous about treatment, discuss sedation with our team ahead of time. Options range from mild oral sedation to deeper techniques where appropriate and safe. We’ll review benefits and considerations so you can make an informed choice that matches your comfort level.
Surgical extractions are required for teeth that are broken at the gumline, ankylosed (fused to bone), impacted, or otherwise inaccessible. In these cases, a small incision and carefully controlled removal of a bit of bone may be necessary to free the tooth. These procedures are performed with local anesthetic and, if indicated, sedation—some complex cases are referred to an oral and maxillofacial surgeon for specialized care.
Because surgical extractions can be more involved, we provide specific pre- and post-operative instructions designed to support healing. These directives cover medication use, activity restrictions, and signs to watch for so that recovery proceeds smoothly.
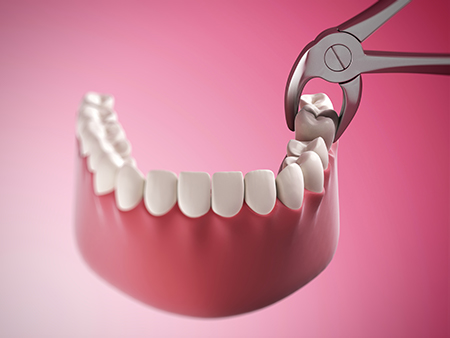
Healing after an extraction is a process that begins immediately. In most straightforward cases, initial healing of the soft tissues occurs within a week, while the deeper bone can continue remodeling for several months. Following your post-op instructions carefully reduces the risk of complications and supports a comfortable recovery.
We provide tailored guidance for each patient, including activity recommendations, dietary suggestions, and pain-control strategies. If you have underlying health conditions or take medications that affect healing, we’ll coordinate care with your medical providers and adapt instructions accordingly.
Good communication is important after surgery. If anything feels unusual—such as increasing pain, persistent swelling, or troubling symptoms—contact our office so we can evaluate and provide timely care. Early attention to concerns helps prevent minor issues from becoming major problems.
Maintaining gauze pressure
Immediately after the extraction, a gauze pad will be placed over the site to encourage a protective blood clot to form. Bite gently and keep firm pressure for the time recommended. Change the gauze only as instructed; if heavy bleeding persists beyond the first few hours, contact our office.
Protect numb tissues
While local anesthesia is active, avoid chewing, and be careful not to bite your lips, cheeks, or tongue. Numbness can linger for a few hours, so take precautions until sensation returns.
Take medications as directed
Antibiotics:
If antibiotics have been prescribed, take the full course exactly as directed to reduce infection risk.
Pain management:
Begin pain medication before the anesthetic fully wears off if advised. Over-the-counter options can offer relief for many patients; follow dosing guidance and only use prescription pain medicines as prescribed.
Protect the forming clot
Avoid rinsing vigorously, spitting, or using straws for the first 24–48 hours so the blood clot can stabilize. Disturbing the clot increases the chance of a painful condition called dry socket.
Use ice to control swelling
Applying an ice pack to the cheek in 10-minute intervals during the first 24 hours can reduce swelling. Keep ice over the area intermittently and follow any personalized instructions from the team.
Avoid smoking
Smoking and using tobacco products interferes with clot formation and healing. Refrain from all tobacco use for at least the first week after surgery to support recovery.
Choose gentle foods
Stick to soft, lukewarm foods and beverages for the first few days. Avoid hot, spicy, or carbonated items, and be sure to stay well hydrated with non-carbonated liquids.
Brush carefully
Maintain oral hygiene but be gentle near the extraction site. After the initial 24 hours, a mild saltwater rinse can help keep the area clean; avoid vigorous swishing.
Keep follow-up appointments
If sutures were placed or additional monitoring is recommended, attend the scheduled return visit so we can confirm that healing is progressing as expected.
If you notice persistent or worsening bleeding, increasing pain, fever, or any unusual symptoms, reach out to our office so we can assess and address the issue promptly.
Preventing issues after an extraction begins with following aftercare instructions but also with planning what comes next for your smile. Where a tooth has been removed for health reasons, we discuss appropriate timing and options for replacement when needed to preserve chewing function and prevent shifting of adjacent teeth.
Common replacement choices include removable dentures, fixed bridges, and dental implants—each has advantages depending on your oral health, bone levels, and long-term goals. We’ll explain the benefits of each and how they fit into a comprehensive plan designed for lasting oral function and aesthetics.
Regular dental visits and maintaining strong home care are important to prevent future problems that could affect remaining teeth. Our goal is to help you keep a functional, comfortable smile and to intervene early if new concerns develop.
You deserve dental care that combines clinical expertise with respect for your comfort and time. At Riverbend Family Dental, we take a measured, patient-centered approach to extractions—prioritizing minimally invasive techniques when possible, thoughtful pain management, and clear recovery guidance so you know what to expect.
We coordinate with specialists when cases require advanced surgical care and provide personalized plans for tooth replacement when needed. Our emphasis is on predictable outcomes, guided by experience and a commitment to gentle, respectful care.
To learn more about what to expect or to discuss whether an extraction is the right step for you, please contact us for more information.

A tooth extraction is the dental procedure used to remove a permanent or primary tooth from its socket in the jaw. Extractions are performed when a tooth cannot be preserved by restorative or endodontic care or when it threatens surrounding teeth and tissues. Treatment is planned after a clinical exam and appropriate imaging to determine the safest, least invasive approach.
Simple extractions are performed on fully erupted teeth that are visible in the mouth and can usually be removed with forceps after local anesthesia. Surgical extractions involve making a small incision, removing bone, or sectioning the tooth when access is limited, such as with impacted wisdom teeth. Your dentist will explain which technique applies to your case and why it offers the best outcome.
Extraction may be recommended for severely decayed teeth that cannot be restored, advanced gum disease that has compromised bone support, or fractures that extend below the gumline. Other reasons include problematic or impacted wisdom teeth, over-retained baby teeth, and cases where extraction is part of an orthodontic plan. The decision is based on a thorough exam, review of X-rays, and consideration of your overall health and treatment goals.
Dentists will discuss alternative treatments when feasible—such as root canal therapy, crowns, or periodontal care—and explain why extraction is the most responsible option for your specific situation. When extraction is chosen, planning includes anesthesia options, a post-operative care plan, and discussion of replacement choices when appropriate. This process helps protect oral health, relieve pain, and prevent further complications.
A simple extraction is performed on a tooth that is fully erupted and accessible in the mouth; the dentist numbs the area and uses instruments to loosen and remove the tooth. These procedures are typically quick and have predictable recoveries when patients follow post-operative instructions. Local anesthesia is usually sufficient for comfort during a simple extraction.
Surgical extractions are needed when a tooth is broken at the gumline, impacted, ankylosed, or otherwise inaccessible without additional steps. They often require a small incision, removal of minimal bone, or sectioning of the tooth to allow safe removal under anesthesia. Complex cases may be referred to an oral and maxillofacial surgeon to ensure specialized care and optimal outcomes.
During the procedure, local anesthesia is used to numb the area so patients should not feel pain, although pressure and movement may be noticeable. For those with anxiety or complex surgical needs, sedation options can provide additional comfort and reduce awareness of the procedure. Before treatment, your dental team will review anesthesia choices and what to expect so you feel informed.
After the extraction, some soreness, swelling, and minor bleeding are normal as tissues begin to heal, and these symptoms typically improve over several days. Following prescribed or recommended pain control strategies, rest, and activity modifications helps keep discomfort manageable. If pain increases after the first few days, or other concerning symptoms develop, contact the office for evaluation to rule out complications.
Sedation choices typically include local anesthesia, nitrous oxide (laughing gas), oral sedation, and, in certain cases, intravenous sedation depending on medical suitability and the complexity of the procedure. Nitrous oxide is useful for mild to moderate anxiety and allows a quick recovery, while oral or IV sedation provides deeper relaxation for more involved care. Your dentist will discuss which options are safe and appropriate based on your medical history and comfort needs.
Be sure to disclose all medications, medical conditions, and prior reactions to anesthesia during your appointment so the team can plan sedation safely. If you are scheduled for sedation at Riverbend Family Dental, arrange for a responsible adult to drive you home and follow any pre-appointment fasting or medication instructions provided. Clear communication about your health and transportation needs helps ensure a safe, comfortable experience.
Preparation begins with a complete medical and dental history review; tell your dentist about prescription medications, over-the-counter drugs, supplements, and any chronic conditions. This information guides decisions about antibiotics, anesthesia, and whether coordination with your physician is necessary. Imaging and a focused clinical exam help plan the most appropriate technique for removal.
If you will receive sedation, follow fasting instructions and avoid alcohol the day before the procedure to reduce risks. Arrange transportation and plan for a period of rest after the appointment, and wear comfortable clothing to your visit. If you have specific concerns or recent changes in your health, contact the office before your appointment so the team can adjust the plan as needed.
Initial soft-tissue healing usually occurs within the first week, but deeper bone remodeling continues for several months as the socket fills in. You may experience swelling, mild bruising, and varying levels of soreness that typically peak within 48 to 72 hours and then gradually improve. Keeping the head elevated, applying ice intermittently during the first day, and resting helps control swelling and discomfort.
Follow post-operative instructions closely—maintaining gauze pressure, avoiding strenuous activity, and choosing soft foods supports proper clot formation and healing. After 24 hours, gentle saltwater rinses can aid cleanliness once advised by your dentist, and you should resume careful brushing while avoiding direct trauma to the site. If bleeding is heavy, pain worsens, or you develop fever or persistent swelling, contact the office promptly for assessment.
Protecting the forming blood clot is the single most important step to avoid dry socket; avoid spitting, swishing forcefully, using straws, and smoking for at least the first week. Follow gauze and wound-care instructions exactly, and take medications as directed to control infection and pain when prescribed. Keeping activity gentle and avoiding vigorous mouth rinsing in the early phase also supports clot stability.
If you notice a sudden increase in pain several days after the extraction, a foul taste, or exposed bone at the site, contact the practice right away for an evaluation. Early attention allows targeted treatment that can reduce discomfort and promote healing. Your dental team will guide you through appropriate interventions and follow-up care when needed.
You can begin eating soft, nutrient-rich foods as tolerated after the procedure and should avoid hot, spicy, or crunchy items for the first few days to prevent irritation. Chew on the opposite side of the mouth while the extraction site heals and progress to firmer foods as comfort allows. Staying hydrated and maintaining a balanced intake supports healing and general well-being.
Resume gentle oral hygiene the day after surgery by brushing your teeth carefully and using a mild saltwater rinse as recommended, avoiding direct pressure on the extraction site. Refrain from heavy exercise or activities that significantly raise your blood pressure for 24 to 48 hours, since increased exertion can prolong bleeding or swelling. Your dentist will provide personalized timing for returning to full activity based on the complexity of your extraction and your recovery progress.
Replacement options include dental implants, fixed bridges, and removable partial dentures, each with advantages depending on the location of the missing tooth, bone levels, and overall oral health. Dental implants provide a stable, long-lasting foundation for replacement teeth when sufficient bone is present, while bridges and dentures offer other predictable solutions for restoring function and appearance. Your dentist will evaluate oral health, discuss the pros and cons of each option, and recommend a timing plan that reflects healing needs and treatment goals.
Planning for tooth replacement is part of comprehensive care, and coordination among your dental providers helps achieve predictable outcomes. Riverbend Family Dental guides patients through the decision process, explains restoration steps, and outlines the healing timeline before definitive work begins. When appropriate, the team will coordinate with specialists to ensure the replacement integrates well with your bite and long-term oral health.

Ready to transform your dental experience?
At Riverbend Family Dental, our team makes achieving optimal oral health easy and stress-free. From routine check-ups to treatments like Invisalign, we provide clear communication and patient-focused care every step of the way.
Getting started is simple—call, email, or use our online portal to schedule a visit and have your questions answered by our experts. Don’t wait—contact Riverbend Family Dental today and experience compassionate, precise care for your smile.