Missing teeth affect millions of people and can change how you eat, speak, and smile. Advances in implant dentistry have made it possible to replace lost teeth with restorations that not only look natural but function like the teeth they replace. Implant therapy focuses on restoring form and function while protecting surrounding oral structures, allowing patients to regain everyday comforts and confidence.
Dental implants are titanium or ceramic posts surgically placed into the jaw to replace missing tooth roots. Once the implant bonds with bone — a process called osseointegration — it serves as a stable foundation for crowns, bridges, or overdentures. That root-level support is what sets implants apart from traditional removable appliances and makes many long-term restorative options possible.
At Riverbend Family Dental, we emphasize personalized treatment planning so each implant solution matches the patient’s needs and goals. Whether the priority is chewing efficiency, speech, or the cosmetic appearance of the smile, contemporary implant restorations can be tailored for predictable outcomes that preserve oral health and facial contours.

While fixed bridges and conventional dentures continue to help many people, implants offer distinct advantages because they integrate with the jawbone. That integration prevents the bone loss that commonly follows tooth extraction, helping to maintain facial structure over time. Implants also remove the need to alter adjacent teeth—something required when preparing a bridge—so they preserve more of your natural dentition.
For patients who currently wear removable dentures, implants can dramatically improve retention and comfort. Simple attachments or fully fixed implant-supported prostheses reduce movement and the need for adhesives, making meals and conversation easier and more enjoyable.
Choosing the right restorative pathway depends on many factors: the number of missing teeth, the condition of surrounding teeth, bone volume, and personal preferences around maintenance and longevity. A careful evaluation establishes which approach will deliver the most natural-looking, functional, and durable result.
Implants are designed to act like the root of a tooth. After placement, the surrounding bone remodels and bonds to the implant surface, creating a strong union. Once healed, the implant supports a prosthetic tooth that sits above the gumline and is shaped, colored, and textured to match adjacent teeth.
The materials and manufacturing techniques used in implant dentistry have improved dramatically over recent decades. Today’s crowns and bridges are crafted from materials that resist staining and wear, while implant components are engineered to provide a reliable connection between the bone and the restoration for years of service when cared for properly.
Good home care and regular dental visits are essential to the long-term success of implant-supported restorations. With appropriate hygiene and monitoring, many patients enjoy stable function and aesthetics that last for decades.
Implant dentistry isn’t one-size-fits-all. There are implant solutions for a single missing tooth, several adjacent missing teeth, or a full arch that needs replacement. Treatment can be restorative (replacing crowns or bridges) or prosthetic (stabilizing dentures), and the ideal option is selected based on clinical findings and the patient’s priorities.
Single-tooth implants restore a missing tooth without altering neighboring teeth. For several consecutive missing teeth, an implant-supported bridge can replace multiple teeth while preserving nearby natural teeth and supporting bone. For patients missing all or most teeth, full-arch implant solutions provide fixed or removable options that restore function and facial support more effectively than conventional dentures.
Advances in digital planning and guided surgery allow clinicians to visualize the final restoration before surgery and place implants with a high degree of precision. This planning improves predictability and simplifies communication between surgical and laboratory teams so the final prosthesis fits and functions as intended.
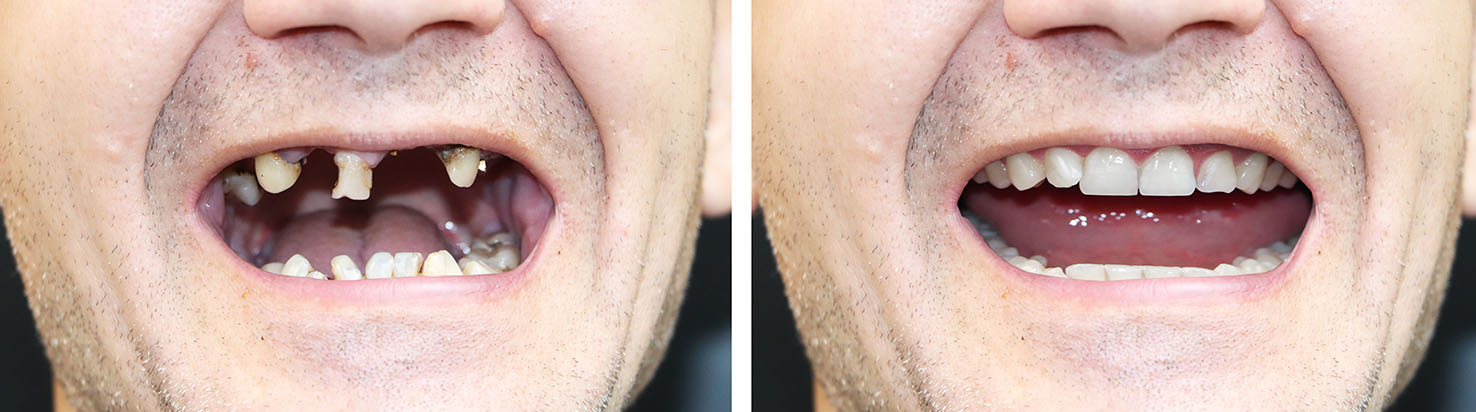
Before any implant is placed, a thorough evaluation determines whether the jaw has adequate bone, the gums are healthy, and there are no untreated sources of infection. This visit typically includes a clinical exam, digital X-rays or 3D imaging, and a review of medical history to ensure safe, coordinated care.
Treatment planning often involves digital models and virtual placement to determine optimal implant size and position. When bone volume is sufficient and no preparatory procedures are required, implant placement can be straightforward. In other cases, additional steps such as grafting or sinus modification may be recommended to create a long-lasting foundation.
Surgery to place implants is commonly performed under local anesthesia and can be completed in one appointment for many patients. We discuss anesthesia options and comfort measures in advance so you know what to expect. After placement, healing is monitored as the implant integrates with bone; that phase typically takes several weeks to a few months, depending on individual healing and the type of restoration planned.
Once implants are placed, the healing phase allows for osseointegration — the biological bonding that gives implants their strength. Some workflows allow for temporary teeth to be attached the same day, offering immediate cosmetic benefit, while other approaches wait for full integration before fabricating the final restoration to ensure a stable long-term result.
Throughout treatment, clear communication keeps patients informed about post-operative care, diet recommendations, and follow-up visits. Careful monitoring and timely adjustments help smooth recovery and prepare for the final restorative phase, when crowns, bridges, or overdentures are securely attached to the integrated implants.
Strong bone and healthy gums are fundamental to predictable implant outcomes. When bone has been lost due to extraction, infection, or long-term tooth absence, placing an implant without augmentation can compromise stability. Fortunately, modern bone grafting techniques can rebuild the jaw and create a reliable foundation for implants.
Grafting materials may be taken from the patient, from donor sources, or use synthetic alternatives, and are chosen based on clinical needs. In many cases bone grafting is performed at the time of extraction or prior to implant placement to restore volume and shape to the ridge, helping achieve a stable, esthetic result.
Other procedures, such as ridge preservation or sinus augmentation, address specific anatomical challenges in the upper jaw. When these adjunctive treatments are needed, they are planned carefully so that implant placement and final restorations meet functional and cosmetic goals while minimizing risk.
Not every implant case needs a graft, but when it does, grafting is a well-established, evidence-based approach to improving long-term success. The decision to graft is made after clinical assessment and imaging, with consideration given to timing, material choice, and the patient’s overall health. With the right preparation, implants can achieve survival rates well above 90% in many clinical studies.
Successful implant therapy combines technical skill, careful planning, and ongoing maintenance. A collaborative approach between the restorative dentist, any surgical specialists, and dental laboratory technicians helps ensure that the implant and its restoration meet expectations for fit, function, and appearance.
At Riverbend Family Dental, we prioritize clear communication and evidence-based techniques to guide patients through every stage — from initial consultation to the delivery of the final restoration and long-term follow-up. Our team focuses on practical advice for hygiene, regular checkups, and early detection of issues so your implant-supported restoration continues to perform well.
Choosing implant therapy is an investment in oral health and quality of life. With modern materials, digital tools, and careful clinical protocols, implants offer one of the most reliable ways to replace missing teeth and protect the surrounding structures for years to come.
Begin with a consultation to discuss your goals, medical history, and the clinical findings that will guide treatment. A personalized plan outlines recommended procedures, expected timelines, and home-care steps to support healing. If implants are appropriate for your situation, a phased approach helps make the process predictable and manageable.
To learn more about implant dentistry and whether it might be the right option for your smile, please contact us for more information. Our team is happy to answer questions and help you understand the best path forward for restoring comfort, function, and confidence.

Dental implants are small titanium or ceramic posts surgically placed into the jaw to replace missing tooth roots. After placement the implant bonds with the surrounding bone through osseointegration, creating a stable base for a prosthetic tooth. This root-level support restores chewing function and helps maintain facial structure.
Once integration is complete, the implant receives a custom crown, bridge, or overdenture that sits above the gumline and is shaped and shaded to match natural teeth. Modern materials and digital workflows improve fit, esthetics, and long-term durability. At Riverbend Family Dental, we emphasize personalized planning so each restoration meets a patient’s functional and cosmetic goals.
Good candidates have healthy gum tissue, adequate jawbone volume, and no uncontrolled systemic conditions that could impair healing. Conditions such as diabetes, smoking, or certain medications may require medical coordination but do not automatically rule out implants. A comprehensive evaluation including medical history, oral exam, and imaging determines candidacy and any preparatory steps.
For patients with insufficient bone, augmentation procedures or alternative prosthetic designs can make implant therapy possible in many cases. Age alone is not a contraindication; treatment decisions focus on overall health, oral hygiene, and realistic expectations. A dental team will discuss benefits and risks and tailor recommendations to individual needs.
Implant solutions range from single-tooth restorations to full-arch fixed prostheses and removable overdentures, each designed to address different patterns of tooth loss. Single implants replace individual teeth without altering neighboring teeth, while implant-supported bridges and fixed full-arch restorations can restore multiple adjacent teeth or an entire arch. Implant-retained dentures improve retention and comfort for denture wearers while remaining removable for hygiene.
The choice of restoration depends on factors such as the number of missing teeth, bone quality, esthetic goals, and maintenance preferences. Digital planning and collaboration with dental laboratories allow clinicians to design prostheses that balance function and appearance. Your clinician will explain the pros and cons of each option and recommend the most predictable solution for your situation.
Preparation begins with a thorough clinical exam, digital X-rays or 3D imaging, and a review of your medical history to identify any factors that could affect treatment. The dental team will evaluate gum health, discuss tobacco use and medications, and order any necessary medical clearances or bloodwork in coordination with your physician. Clear communication about your health goals and concerns helps form a safe, individualized treatment plan.
On the day of surgery you will receive instructions about eating, medications, and arrival times to help the appointment go smoothly. Local anesthesia is commonly used and additional comfort measures are discussed in advance to address anxiety or specific medical needs. After the procedure, the team will provide detailed post-operative care guidance and schedule follow-up visits to monitor healing.
The timeline varies with each case but commonly includes implant placement, a healing interval for osseointegration, and attachment of the final restoration. Healing can take several weeks to a few months depending on bone quality, the need for grafting, and whether immediate temporary restorations are placed. Some workflows allow provisional teeth the same day, while others wait for full integration to maximize long-term stability.
Throughout this process, periodic checkups and imaging ensure the implant is integrating properly and the soft tissues are healthy. Adjustments to provisional restorations and refinement of occlusion prepare the mouth for the final crown, bridge, or denture. Your clinician will provide an estimated schedule based on clinical findings and keep you informed at each stage.
Bone grafting is recommended when there is insufficient jawbone height or width to support an implant safely and predictably. Grafting materials may be sourced from the patient, donor tissue, or synthetic substitutes, and they are selected based on the clinical situation and treatment timeline. When performed properly, grafts can restore volume and create a stable foundation for later implant placement.
Sinus augmentation addresses bone loss in the upper posterior jaw by gently elevating the sinus floor and placing graft material to increase vertical height. These procedures often add time to the overall treatment plan because grafted sites require a healing period before implants are placed or loaded. Your dentist will explain whether augmentation is needed and discuss the expected healing milestones and follow-up care.
Like any surgical procedure, implant placement carries risks such as infection, temporary swelling, and rare instances of nerve or sinus involvement. Careful treatment planning, aseptic technique, and adherence to post-operative instructions reduce these risks and support predictable healing. Early signs of complications are monitored at follow-up visits so they can be addressed promptly.
If an issue arises, management options range from conservative measures such as medication and local care to more advanced interventions coordinated with surgical specialists when necessary. Long-term success relies on good oral hygiene, routine monitoring, and timely attention to changes in function or comfort. Your dental team will discuss potential complications during the consultation and outline contingency plans tailored to your case.
Implants restore a tooth at the root level, which helps preserve bone and facial contours in ways that bridges and conventional dentures cannot. Bridges require reshaping adjacent healthy teeth for support, whereas implants often preserve natural tooth structure. Removable dentures can restore appearance and chewing ability but may lack the stability and bone-preserving benefits of implants.
For denture wearers, implant attachments or fixed prostheses can markedly improve retention, comfort, and chewing efficiency without the need for adhesives. Decision-making considers the number of missing teeth, bone availability, hygiene demands, and long-term maintenance expectations. A clinical evaluation helps determine which restorative pathway best balances durability, function, and the patient’s everyday needs.
Maintaining implant health requires consistent home care practices such as brushing twice daily, cleaning around implants with interdental tools recommended by your dentist, and avoiding habits that stress the restoration. Regular professional cleanings and exams allow clinicians to assess soft tissue health, check for early signs of peri-implant inflammation, and perform necessary maintenance. Using the correct instruments and techniques helps protect both the implant and surrounding natural teeth.
Patients should report any changes in comfort, mobility, or bite as soon as they occur so issues can be evaluated early. Periodic radiographs and clinical probing may be part of the monitoring protocol to confirm bone stability and tissue health. With attentive care and routine follow-up, many implant restorations provide reliable function for many years.
Riverbend Family Dental uses evidence-based protocols, digital imaging, and coordinated care to develop individualized implant plans that reflect each patient’s goals and oral health needs. The team emphasizes clear communication, letting patients understand the clinical findings, recommended procedures, and expected recovery so they can make informed decisions. Collaboration with surgical colleagues and dental laboratories ensures the technical and esthetic aspects of the restoration are addressed.
Before treatment begins the practice conducts a comprehensive evaluation including 3D imaging when appropriate to assess bone, adjacent teeth, and anatomic considerations that affect implant placement. Treatment plans outline sequencing, expected timelines, and hygiene guidance to support healing and long-term success. Follow-up care and routine maintenance help protect your investment in oral function and appearance.

Ready to transform your dental experience?
At Riverbend Family Dental, our team makes achieving optimal oral health easy and stress-free. From routine check-ups to treatments like Invisalign, we provide clear communication and patient-focused care every step of the way.
Getting started is simple—call, email, or use our online portal to schedule a visit and have your questions answered by our experts. Don’t wait—contact Riverbend Family Dental today and experience compassionate, precise care for your smile.