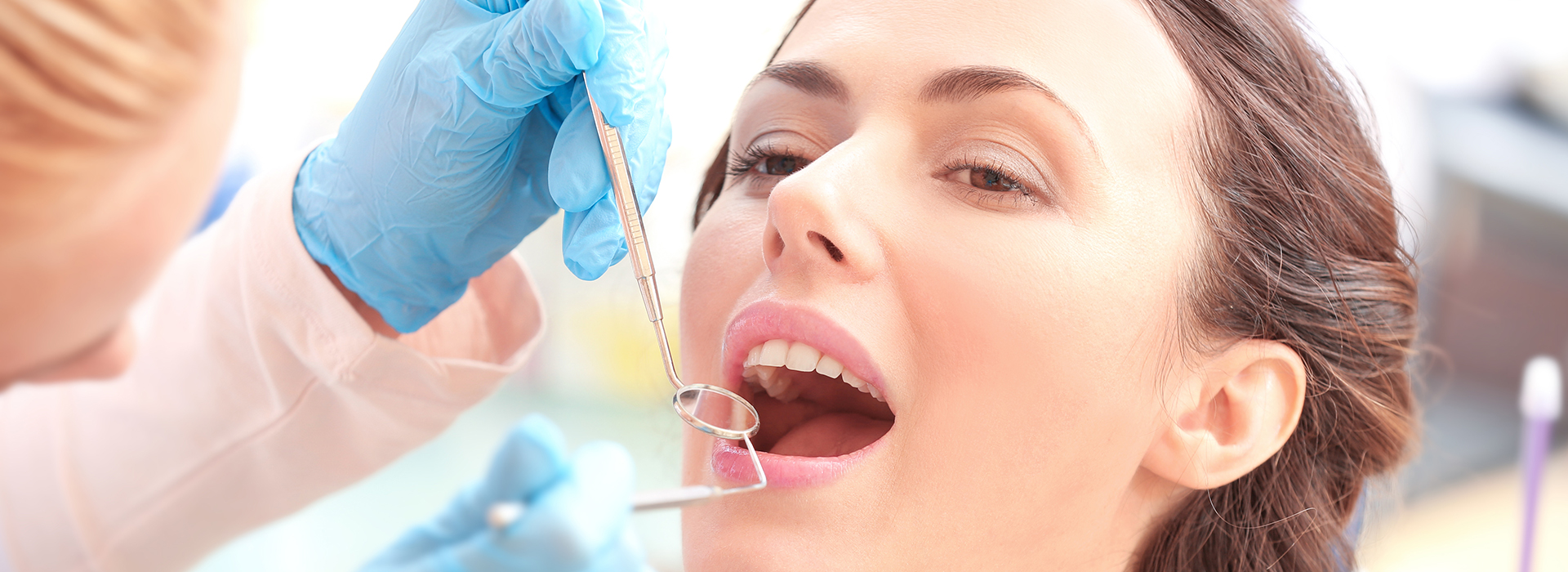
Gum disease is one of the most common threats to adult oral health — and it often advances quietly. Studies show that many adults experience some form of periodontal inflammation during their lifetime. At the office of Riverbend Family Dental, we focus on early detection and practical treatment strategies so patients can preserve natural teeth and maintain comfortable, functional smiles.
This page outlines how gum disease develops, what to watch for, and the range of modern treatments available. Our aim is to give you clear, useful information so you can make informed decisions about your periodontal care.
Gum disease begins with dental plaque: a sticky biofilm teeming with bacteria that forms on tooth surfaces. If plaque remains in place, it hardens into tartar (calculus) and irritates the gum tissue. That irritation triggers an inflammatory response — the process we recognize as periodontal disease.
In many cases the earliest stages are painless. Gums may look slightly red or swell a bit before any discomfort appears, which is why routine dental exams and cleanings are essential. Your dental team can spot subtle changes before the condition advances.
Recognizing the warning signs helps you act early. Common indications of gum disease include swollen or tender gums, bleeding when you brush or floss, persistent bad breath, and gums that appear to be pulling away from the teeth. If you notice these changes, schedule an evaluation promptly.

Healthy gums do more than protect your smile — they help maintain overall well-being. Researchers have identified links between periodontal inflammation and several systemic conditions, including diabetes and cardiovascular disease. While those connections are complex and still under study, reducing oral inflammation is a sensible part of staying healthy.
Controlling gum disease helps preserve the jawbone and surrounding tissues that support each tooth. When periodontal problems escalate, the loss of supporting tissues can create long-term functional and aesthetic consequences that are harder to reverse.
Prevention and maintenance are the most effective strategies: consistent home care, regular professional cleanings, and early treatment when problems are detected. Together, these steps reduce bacterial buildup, slow tissue breakdown, and protect both oral and overall health.
Gingivitis is the reversible, initial phase of gum disease. It shows up as redness, slight swelling, and bleeding during brushing or flossing. Because it usually does not cause pain, many people are unaware they have it until a clinician points it out.
The encouraging news is that gingivitis is often completely reversible with improved oral hygiene and professional care. An individualized plan that includes effective brushing and interdental cleaning, along with more frequent cleanings, can bring inflammation under control and return the tissues to health.
Your dental team will recommend the best follow-up schedule based on your response to treatment. For most patients, consistent home care plus periodic professional cleanings prevents recurrence and keeps gingivitis from progressing to more destructive stages.

Left untreated, gingivitis can evolve into periodontitis, a condition in which the inflammation extends beneath the gumline and begins to damage the bone and connective tissues that anchor teeth. This process creates pockets around teeth where bacteria accumulate and continue to fuel tissue breakdown.
As pockets deepen and supporting bone is lost, teeth can feel loose, spacing can change, and chewing may become uncomfortable. At this stage, reversing the damage is more challenging; the focus shifts to halting progression, stabilizing the dentition, and, where appropriate, restoring lost tissue.
Effective management depends on an accurate diagnosis and an individualized plan that addresses both the bacterial cause and the structural consequences of disease. With modern periodontal care, many patients can halt progression and regain a healthy, manageable condition.
Diagnosis begins with a careful clinical exam and periodontal charting to measure pocket depths, assess gum attachment, and identify areas of bone loss on dental X-rays. We also review your overall health, medications, and lifestyle factors that influence healing and disease risk.
Treatment plans are tailored to the severity and pattern of disease. Early-stage disease is often managed with improved hygiene and deeper professional cleanings known as scaling and root planing. More advanced conditions may require adjunctive therapies — local antimicrobials, systemic medications when indicated, or surgical approaches to reduce pocket depth and restore healthy anatomy.
Throughout treatment, the goal is to reduce the bacterial burden, control inflammation, and create conditions that allow the tissues to remain stable with routine maintenance. Long-term success depends on the combination of professional care and consistent home hygiene.
When disease is caught early or is localized, conservative care is the first step. Scaling and root planing — a focused deep cleaning beneath the gums — removes plaque and hardened deposits from root surfaces and helps the tissue heal.
These procedures are often combined with improved home care instructions and may include targeted antimicrobial agents placed near affected roots. The objective is to reduce pocket depth, lower bacterial levels, and stop inflammation without surgery whenever possible.
Many patients respond well to this approach and can maintain periodontal health with a personalized maintenance schedule. If results are incomplete, the care team will discuss additional options designed to protect long-term oral function.
When pockets are deep or bony defects are present, surgical interventions are sometimes necessary to access infected root surfaces, reshape damaged tissues, and stabilize the area. Flap procedures allow direct cleaning and recontouring of bone and soft tissues to create a healthier environment for maintenance.
Regenerative techniques — such as bone or soft tissue grafting and membrane-guided regeneration — aim to rebuild lost supporting structures when appropriate. In selected cases, laser-assisted therapies are used to reduce diseased tissue and improve healing.
The shared goal of surgical and regenerative treatment is to restore a stable architecture that patients can maintain with routine care, reducing the risk of further tooth loss and improving comfort and function.
At Riverbend Family Dental, our approach blends proven clinical techniques with a focus on patient education and long-term maintenance. If you have concerns about bleeding gums, loose teeth, or changes in your bite or smile, please contact us for more information about periodontal evaluation and care.

Periodontal disease is an infection and inflammation of the gums and the structures that support the teeth, including the periodontal ligament and alveolar bone. It begins when bacteria in dental plaque provoke an immune response that damages soft tissue and, in advanced cases, the jawbone. Early stages are often reversible, but progressive disease can lead to irreversible bone loss and tooth mobility.
Gum disease typically progresses along a spectrum from gingivitis to periodontitis, with clinical signs becoming more pronounced as the condition advances. Gingivitis affects only the soft tissues and is usually reversible with improved hygiene and professional care. Periodontitis involves deeper pockets and tissue destruction and requires targeted periodontal treatment to control the infection and stabilize the dentition.
The primary cause of gum disease is the accumulation of bacterial biofilm, or plaque, on tooth surfaces and along the gumline. Contributing factors include smoking, poorly controlled diabetes, certain medications, hormonal changes, genetics, poor oral hygiene, and a history of periodontal problems. These factors can alter the immune response or encourage faster plaque accumulation, increasing the likelihood of disease progression.
Age and systemic health also influence risk, with older adults and people with chronic conditions more likely to experience advanced disease. Lifestyle choices such as tobacco use and inadequate oral care further raise risk. Understanding and managing these factors helps clinicians create a personalized prevention and treatment plan.
Common early signs include red, swollen, or tender gums and bleeding during brushing or flossing. As disease progresses, patients may notice persistent bad breath, gum recession, formation of deep pockets between teeth and gums, and looseness or shifting of teeth. Symptoms can be subtle, so the absence of pain does not rule out active disease.
Because some patients do not experience obvious symptoms until later stages, routine dental exams are essential for early detection. Dental professionals use visual inspection, periodontal probing and radiographs to identify hidden inflammation and bone loss. Timely diagnosis increases the chances of controlling the disease with less invasive therapy.
Diagnosis begins with a thorough clinical exam that includes measuring pocket depths around each tooth, assessing bleeding on probing and checking for gum recession and tooth mobility. Dental radiographs are used to evaluate underlying bone levels and detect patterns of bone loss that are not visible clinically. A detailed medical and dental history helps identify systemic or medication-related contributors to periodontal disease.
Periodontal charting creates a baseline record to guide treatment and track progress over time. In some cases, your dentist may refer you to a periodontist for advanced assessment or specialized care. Regular reassessment following treatment ensures the chosen approach is effectively controlling inflammation and protecting supporting structures.
The cornerstone of non-surgical therapy is professional mechanical debridement, commonly called scaling and root planing, which removes plaque and tartar from above and below the gumline and smooths root surfaces to discourage bacterial recolonization. This treatment is often combined with improved home care, including proper brushing technique, interdental cleaning and antiseptic rinses as recommended. For many patients, these measures reduce pocket depths and resolve inflammation without the need for surgery.
Adjunctive therapies such as locally delivered antimicrobials or prescription rinses may be used selectively to enhance outcomes in areas that respond poorly to mechanical therapy alone. The choice and timing of adjuncts are informed by clinical findings and the patient’s overall health. Regular maintenance visits are essential to sustain improvements achieved with non-surgical care.
Surgical intervention is considered when non-surgical therapy fails to achieve pocket reduction or when there are anatomical defects, persistent deep pockets, or significant bone loss that compromise long-term tooth stability. Common surgical goals include pocket reduction, regeneration of lost bone and attachment, and correction of defects that trap plaque. Types of procedures can include flap surgery for access, bone grafting, guided tissue regeneration and soft tissue grafts to address recession.
The decision to proceed with surgery depends on a comprehensive evaluation of disease severity, patient health, and treatment goals. Surgery aims to create a more maintainable oral environment and improve functional and esthetic outcomes when indicated. Detailed preoperative planning and postoperative maintenance are critical to surgical success and long-term stability.
Most periodontal procedures are performed with local anesthesia to minimize discomfort during treatment, and many patients report only mild to moderate soreness afterward. Discomfort is typically managed with short-term analgesics and cold compresses, and it tends to decrease substantially within a few days. Your dental team will provide specific postoperative instructions to reduce swelling and protect healing tissues.
Recovery varies with the type and extent of treatment, with non-surgical care generally having a quicker return to normal activities and surgical procedures requiring longer healing and temporary dietary adjustments. Maintaining careful oral hygiene and attending follow-up visits are important to support healing and monitor treatment response. If you experience unexpected pain, prolonged bleeding or signs of infection, contact your dental provider promptly for evaluation.
Antibiotics and antimicrobial agents can be effective adjuncts to mechanical cleaning in selected cases, especially when specific pathogenic bacteria are implicated or when infection persists despite debridement. Options include locally delivered antimicrobials placed directly into periodontal pockets, short courses of systemic antibiotics for targeted cases, and antiseptic mouth rinses to reduce bacterial load. These measures are used selectively and are not a substitute for thorough mechanical removal of plaque and calculus.
Your clinician will weigh the benefits and risks of adjunctive antimicrobials based on the clinical presentation, medical history and potential resistance concerns. Cultures or molecular testing are sometimes used to guide targeted therapy in refractory cases. Responsible use of antimicrobials, combined with mechanical therapy and maintenance, offers the best chance for long-term control of periodontal infection.
Prevention after treatment focuses on consistent, effective home care and a regular professional maintenance schedule to control plaque and prevent reinfection. Recommended habits include twice-daily brushing with a soft-bristled brush, daily interdental cleaning with floss or interdental brushes and using an antiseptic rinse if advised by your clinician. Lifestyle changes such as smoking cessation and good control of systemic conditions like diabetes also play a major role in reducing recurrence risk.
Professional periodontal maintenance visits are tailored to the individual and may occur every three months or at an interval determined by disease severity and response to treatment. These visits allow for professional cleaning in areas that are difficult to maintain at home and for early detection of any returning inflammation. Staying engaged with your dental team and following their guidance supports long-term gum health and helps preserve natural teeth.
After active periodontal therapy, many patients benefit from maintenance visits every three months, a cadence that helps control bacterial recolonization and monitor tissue stability. The exact interval is individualized based on factors such as the initial disease severity, response to therapy, systemic health and risk behaviors like smoking. During maintenance appointments, clinicians reassess pocket depths, remove new deposits and reinforce home care techniques.
The practice will establish a personalized recall schedule and adjust it over time according to clinical findings and the patient’s ability to maintain oral hygiene. For complex or refractory cases, collaboration with a periodontist may be recommended to ensure optimal long-term outcomes. Adherence to a recommended maintenance program is one of the strongest predictors of sustained periodontal health.

Ready to transform your dental experience?
At Riverbend Family Dental, our team makes achieving optimal oral health easy and stress-free. From routine check-ups to treatments like Invisalign, we provide clear communication and patient-focused care every step of the way.
Getting started is simple—call, email, or use our online portal to schedule a visit and have your questions answered by our experts. Don’t wait—contact Riverbend Family Dental today and experience compassionate, precise care for your smile.